Managing Psoriasis in Your Ears
March 31, 2023
Content created for the Bezzy community and sponsored by our partners. Learn More
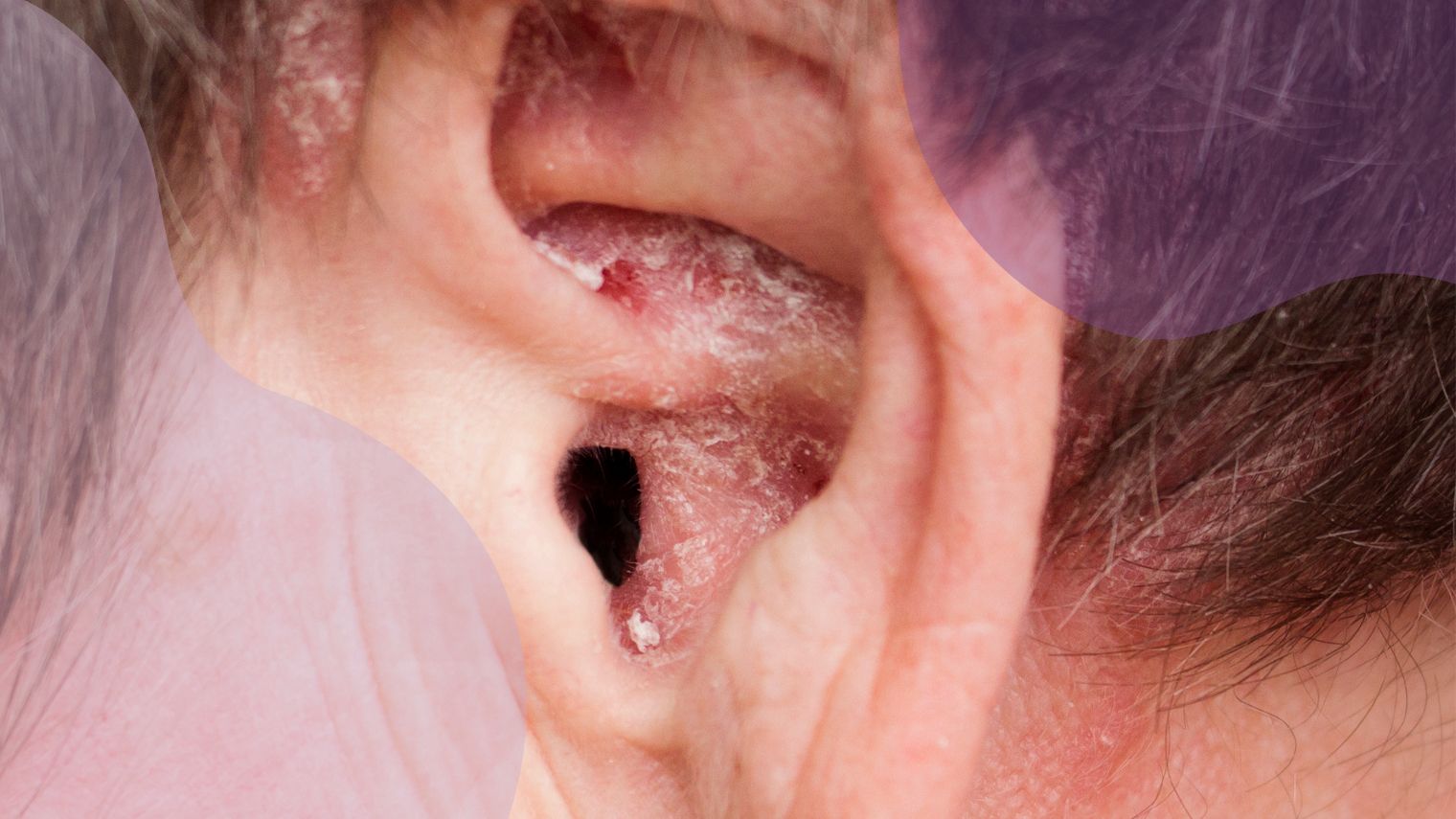
Photography by Lipowski/Getty Images
There are special considerations when dealing with psoriasis in and around your ears. In addition to the possibility of temporary hearing loss, it’s important to use caution and work with a doctor when managing ear psoriasis to prevent damage to the area.
Psoriasis that forms in or around your ears can be itchy and uncomfortable. In some cases, the buildup of scales can lead to temporary hearing loss. You may also feel self-conscious due to the highly visible location.
All these factors can then impact your self-esteem and mental health. But you are far from alone.
A chapter published in 2020 notes that psoriasis on the external ear area is common, with approximately two-thirds of people with psoriasis experiencing plaques on the ear lobes and in the conchal bowl (the cupped area of the ear that is outside of the ear canal).
You can take steps to manage psoriasis in your ears. This can involve treating the lesions, avoiding triggers, and taking care of your mental health needs.


Symptoms
According to a 2019 survey, medical professionals said the most commonly reported symptom of ear psoriasis was pruritus, which is the medical term for itchy skin. Less than 25% of the medical professionals reported patients describing any kind of hearing issue.
But there is a big “but” here. This survey was given to doctors serving on the Medical Board of the National Psoriasis Foundation. Part of the survey’s intention was to understand how doctors approach the diagnosis and treatment of ear psoriasis.
Findings revealed that 75% of respondents did not inspect the ear canal during psoriasis diagnosis. The doctors also noted that during exams, not all of them routinely ask about ear or hearing-related symptoms.
The researchers noted that about 13% of doctors ask about hearing loss. And only about 56% ask about itchiness related to ear psoriasis.
In other words, the true rate and occurrence of symptoms of ear-related psoriasis may not be fully known because doctors are not thoroughly examining or asking about their patient’s ears.
What is known is that psoriasis lesions can and do occur in and around the ears. You may notice it appears:
- behind the ears
- around the ears
- in the ear canal
Because not all doctors ask about hearing loss and itching related to ear psoriasis, tell your doctor if you have these symptoms so you can get help addressing them properly.
Causes
No one really knows why psoriasis may appear in and around the ears. It may happen if you experience scalp or facial psoriasis, may develop over time following plaques on other areas of the body, or your psoriasis may start in the ear area.
Things that are known about the causes of psoriasis include:
- it does not start because you touch your ears too much
- you can’t “catch it” from someone else
- it has nothing to do with cleanliness or hygiene
- triggers can cause it to flare or get worse
You’ve probably heard the term triggers before. Simply put, triggers are anything you come in contact with that cause your psoriasis symptoms to start or get worse.
Triggers can be tricky. They vary from person to person, so what causes your symptoms to get worse may be different from someone else’s.
Still, experts know about a few common triggers that a lot of people react to. They include:
- Stress: One of the most common triggers. You may experience stress from work, family life, school, money, or any number of underlying causes. Psoriasis itself may stress you out.
- Illness: Anything that affects your immune system can trigger psoriasis.
- Injury to the skin: If you accidentally cut your ears or pierce them, it could trigger a psoriasis flare.
- Weather: Changes in the weather, your daily sun exposure, drier air, or other factors can trigger a flare of psoriasis in your ears or other areas.
- Other triggers: Allergies, drinking alcohol, eating certain foods, cosmetic products, and other chemicals can trigger a flare.
It can be helpful to keep a journal to help you track your flares and possible triggers. Ask yourself:
- Do your ears feel worse after using a certain shampoo?
- Do they always flare in the spring?
- Do they get worse after you have a few drinks the night before?
If you write down when they flare as well as things you know were going on at the time, it can help you figure out your triggers and find ways to avoid them.
Scalp psoriasis is a common, yet frustrating, symptom of a psoriasis flare. In addition to being on the scalp, plaques can appear on the hairline, forehead, back of the neck, and around your ears. Having psoriasis plaques on your scalp and nearby areas can be uncomfortable. Scalp psoriasis can also be hard to treat, which can make it particularly distressing.
Joni Kazantis in How Can I Manage Scalp Psoriasis?
Read more: Ask Joni: How Can I Manage Scalp Psoriasis?
Treatment
Treating psoriasis in the ear involves different approaches. Due to the sensitive nature of the skin in the area and the structure of the ear, it’s important to use caution and work with a doctor to determine the best course of action.
It’s likely your plan may involve some or all of the following:
Avoiding triggers
Part of your treatment and management plan can involve identifying and avoiding triggers. Sure, it’s not always possible to avoid triggers but taking some steps may help.
Avoiding triggers is a good first step, in part because ear psoriasis can be a bit tricky to treat.
Using medications
Topical corticosteroids are the most commonly reported first-line treatment for psoriasis in the ear no matter where it appears. Topical means you apply it directly to your skin. Corticosteroids, also known as steroids, provide an anti-inflammatory effect.
A secondary choice for treatment is topical calcineurin inhibitors (TCIs). This type of cream or ointment helps to reduce the immune system’s activity in the affected area.
If topicals do not work, a doctor may recommend trying corticosteroid injections. For injections, you would go to a doctor’s office where they would use a needle to deliver the medication directly to the psoriasis plaques or lesions.
Sometimes doctors recommend the use of biologics to treat psoriasis that appears on or in the ears. Biologics are a type of medication that targets the immune system and reduces its activity. This helps to reduce inflammation in your body, which can help reduce the severity of psoriasis.
Removing plaques
If you find you are having trouble hearing, it could be that the scales have built up in your ear canal. You should not try to remove this yourself.
Sticking your finger or other objects in your ear may push the scale and wax buildup further into the ear.
Instead, if you have hearing loss, you should consider seeing a dermatologist or otolaryngologist. An otolaryngologist is also known as an ear, nose, and throat (ENT) doctor.
Either of these specialists can help remove excessive buildup in your ear. They may recommend irrigating the ear or using drops to help break up the scales and allow them to come out more easily.
If hearing loss persists, it’s important to follow up on care. There is some association between psoriasis and other causes of hearing loss, though the connections are unclear and more research is needed.
Addressing your mental health
An important part of your health is making sure you take care of your mental well-being.
Psoriasis and depression often occur together. A research review in 2020 reports that psoriasis and depression share several underlying mechanisms — like inflammation, melatonin levels, genetics, and low vitamin D3 levels.
Also, fear of social rejection, as well as self-stigmatization about your psoriasis, can fuel symptoms of depression.
If you find you are feeling sad all the time, unmotivated even by things you enjoy, or any other signs of depression, you may want to ask a doctor for recommendations for mental health professionals in your area. They may also suggest other therapies and support groups.
The National Psoriasis Foundation offers several resources and ways to connect with other people with psoriasis. You can get started exploring their peer groups and other support groups here.
The bottom line
Ear psoriasis can cause discomfort, itchiness, and temporary hearing loss in some people. It can be challenging both emotionally and in terms of treatments since options are a bit more limited compared with other areas of the body.
Management can involve a combination of topical therapies, avoiding triggers, and addressing any other mental health concerns. Working with a team of doctors or medical professionals may help.
Medically reviewed on March 31, 2023
8 Sources


Like the story? React, bookmark, or share below:
Have thoughts or suggestions about this article? Email us at article-feedback@bezzy.com.
About the author